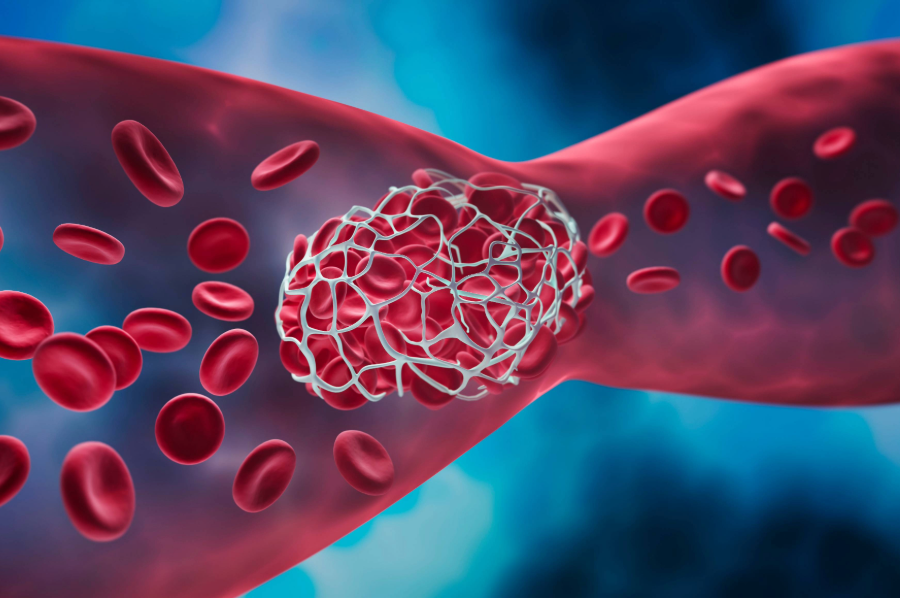
Here in the Lowcountry, we’re familiar with the summer squall, and we know that when debris clogs a storm drain, water swells into the street. With that analogy in mind, let’s take a closer look at the common condition deep vein thrombosis (DVT).
The body contains two venous systems: superficial veins run underneath the skin while deep veins run adjacent to arteries and return blood to the heart.

What’s the holdup?
So, how does this clog form? In the case of our rain drain, leaves, sticks, and dirt may have built up or the sewer may be damaged. The same goes for the body. A DVT can occur if blood stagnates when a person remains in the same position for too long, as well as with a hypercoagulable disorder or abnormality of the vein lining. “That stagnation of blood can happen after an operation or with any medical condition that keeps a patient in bed or a wheelchair,” says the surgeon. “Or it could be from sitting still on a long car or plane ride.”
Like getting caught in the rain, DVTs can happen to anyone. A person’s risk does increase with age, especially after age 30. “But there isn’t a distinct age distribution or gender bias,” adds Dr. Gaillard, who regularly navigates the condition with a variety of patients.
Hypercoagulable disorders, in which blood clots too easily, are rare, impacting only about one in one thousand people.
Clear the way
When a clot hits, “it’s not subtle,” says the doctor, explaining that swelling begins immediately. As such, most people head to the emergency room, where a vascular surgeon will be called in for consultation. If the swelling and pain aren’t severe enough for an ER trip, an urgent visit to a primary care physician will also get treatment moving.
“Diagnosing DVT involves fairly simple tests, such as an ultrasound,” says Dr. Gaillard. From there, the decision to operate or not usually boils down to location. Leg clots can often be eliminated with a three- to six-month course of blood thinning medication along with compression and elevation to address swelling. Iliofemoral clots, which are situated between the groin and inferior vena cava (where the leg veins meet around the belly button), pose a higher risk of complications, giving doctors good reason to operate. Without surgical intervention, iliofemoral clots are more likely to lead to long-term stress on the leg veins (known as post thrombotic syndrome) or the potentially fatal pulmonary embolism.
DVT surgery consists of thrombolysis, in which a catheter delivers clot-busting medication to the site, or thrombectomy, the direct removal of the clot from the blood vessel.
Keep it moving
“What’s hammered home in our medical teaching are the impacts of prolonged sitting and immobility,” stresses Dr. Gaillard. When facing an injury or undergoing any kind of operation, talk to your doctors about how to safely maintain good mobility. And if you’re traveling a long distance, he recommends moving every two hours. “It can be as simple as pedaling your feet in a seated position.”
Roper St. Francis Healthcare leads the Tri-County in innovative healthcare with a compassionate, patient-first approach. The new Roper St. Francis Physician Partners Vascular Surgery practice delivers streamlined care to meet the region’s complex vascular needs and improve the health of the communities we serve. Learn more about our vascular services and locations at rsfh.com/heart-vascular, or connect with our specialists by dialing (843) 720-8448.